Reduce Antibiotic Use In Human Medicine
In 2020, hospital administrators, accrediting organizations, and policymakers should focus on enhancing the quality of hospital antibiotic stewardship programs, which aim to ensure appropriate antibiotic use and patient safety. Thanks to a September 2019 federal rule change, all hospitals participating in Medicare and Medicaid must implement stewardship programs as of March 2020. Because over half of patients receive antibiotics during their stays, this change represents a major step forward in slowing the emergence of antibiotic-resistant bacteria.
Improved antibiotic prescribing is also needed in outpatient health care settings, such as doctors offices, emergency rooms, retail health clinics, and urgent care centers. The Joint Commission, a nonprofit accrediting organization, recently finalized its stewardship requirement for outpatient facilities, an important step in the right direction. Though encouraging, this requirement applies only to the relatively small portion of outpatient clinics the organization accredits.
Wider implementation of meaningful stewardship programs is critical, but that will require concerted action by health insurance plans, health systems, and state and local health agencies. For example, these health care stakeholders can support stewardship efforts by providing antibiotic prescribing feedback to physicians, a method that has proved successful in improving prescribing practices.
How Can I Improve Antibiotic Use
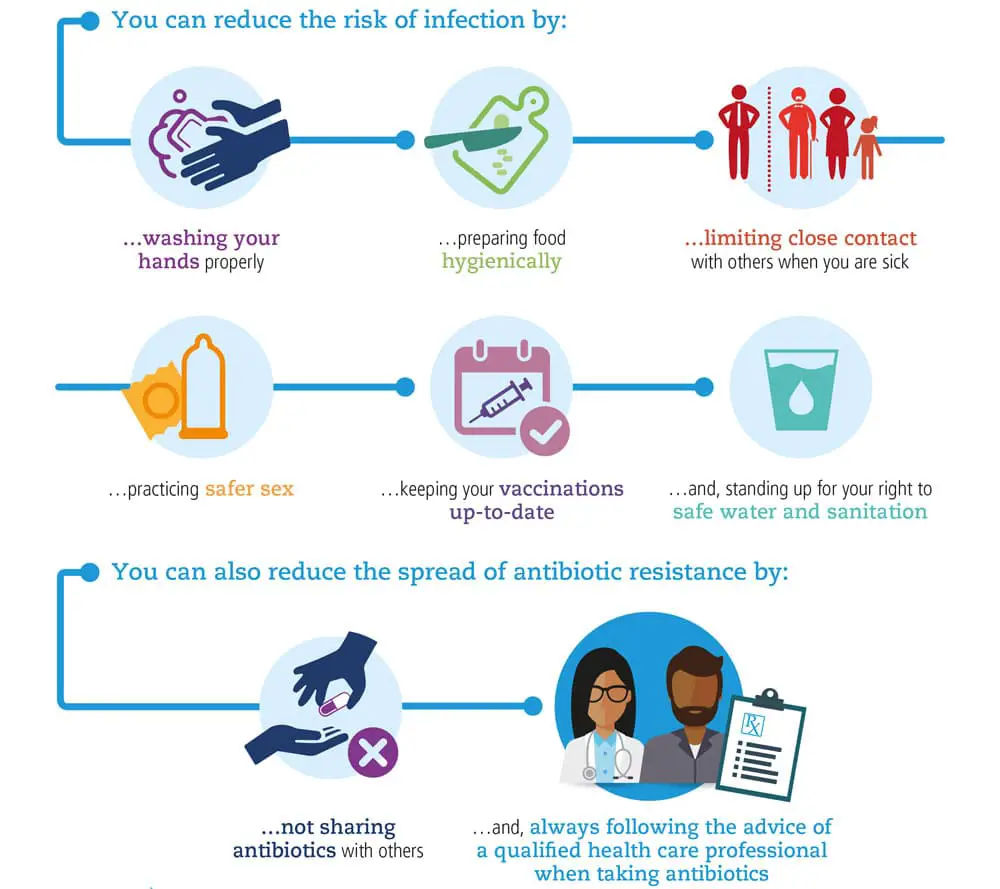
No one can completely avoid getting an infection, but there are additional steps you can take to protect yourself and your family.
Taking antibiotics only when they are needed is an important way you can protect yourself and your family from antimicrobial resistance. Talk to your doctor about the best treatment if you are sick. Never pressure your doctor to prescribe an antibiotic.
When antibiotics arent needed, they wont help you, and their side effects could still cause harm. Ask your doctor or pharmacist about steps you can take to feel better when an antibiotic isnt needed.
If your doctor decides an antibiotic is the best treatment when you are sick:
- Take the medication exactly as your doctor tells you.
- Do not share your medication with others.
- Do not save them for later. Talk to your pharmacist about safely discarding leftover medicines.
- Do not take antibiotics prescribed for someone else. This may delay the best treatment for you, make you even sicker, or cause side effects.
- Talk with your doctor and pharmacist if you have any questions about your antibiotics prescribed to you.
What Do People Know
Numerous epidemiological studies on ABR have been undertaken in high- middle- and low-income countries. Most of these studies have been descriptive using cross-sectional surveys addressing questions such as awareness, knowledge, attitudes and practice.
A study across 12 countries was conducted in 2015 as part of the implementation of objective 1 of the WHO Global Action Plan to improve the awareness and understanding of AMR through effective communication, education and training. The study, which included 9,772 respondents, found that 65% had taken antibiotics during the prior 12 months, and 35% within the last month. The latter figure was 42% in low-income countries and 24% in people aged 65 years and older. Twenty-five percent of people across the 12 countries thought that it was acceptable to use antibiotics left-over from others and 32% reported that they generally stop taking antibiotics when they feel better. Two-thirds of the respondents believed that colds and flu can be cured with antibiotics. Some correct actions, such as regular hand-washing and only taking antibiotics when prescribed were acknowledged. The study revealed major misunderstandings regarding the meaning of ABR. While there was high awareness about increasing ABR , three quarters incorrectly believed that their body, rather than bacteria, become resistant to antibiotics. Many also held the view that it is only a problem for those who take antibiotics regularly .
Don’t Miss: What Kind Of Human Antibiotics Can Dogs Take
What Do Prescribers Know
Prescribing at best occurs through a consultative dialogue between the patient and the doctor. Knowledge and expectations for both come into play. Doctors are expected to be well-informed. However, in a systematic review of 57 published studies, which included almost twelve thousand clinicians, most of which from North America and Europe, 89% recognized ABR as a global problem but only 67% saw it as an issue of relevance for their own practices. In qualitative interviews, doctors acknowledged that ABR was a serious problem, but one caused by others. They saw ABR as a big problem in their own countries, but being of less importance in the hospitals where they work, and not of particular relevance on their clinics .
As part of the implementation of a US campaign to prevent ABR, 695 clinicians took part in surveys, in-depth interviews and focus groups to assess barriers to prevent AMR in healthcare settings . When evaluating the campaign´s four main strategies they ranked Diagnose and treat infection effectively and Use antimicrobials wisely higher than Prevent infection and Prevent transmission .
A study from Ghana in which most prescribers were nurses, showed that knowledge about ABR was high, although there were gaps in the knowledge and perception among different prescriber categories. The interviewees requested more formal information about ABR to support prescribers antibiotic prescription practices .
Minnesotans Can Help Keep Antibiotics Effective By Using Them Properly And Only When Necessary
Mirroring a trend seen nationally, Minnesotas progress toward reducing antibiotic resistance lost ground in recent years, but the Minnesota Department of Health is aiming to work with health care partners to renew and accelerate the push to preserve antibiotic effectiveness.
Following years of reductions in antibiotic-resistant infections, hospital-related resistant infections and deaths increased at least 15% nationally during 2020, the first year of the COVID-19 pandemic, according to a new report from the Centers for Disease Control and Prevention , COVID-19: U.S. Impact on Antimicrobial Resistance. Progress on improving the ways in which antibiotics are used has also taken a step back during the pandemic, according to the report.
The last few years presented many challenges, said Minnesota Commissioner of Health Jan Malcolm. We know that our health care system has been strained and this has contributed to the growth of antibiotic resistance. However, preventing antibiotic resistance is extremely important. We must regain and accelerate the progress we had been making before the pandemic hit. Peoples lives may depend on it.
Antibiotic resistance happens when bacteria germs that cause many serious infections in people become able to resist the medications designed to kill them or slow their growth. Bacteria that become resistant to antibiotic medications can lead to much more severe infections and even deaths that would not otherwise occur.
-MDH-
Recommended Reading: Antibiotics For Uti Bladder Infection
One Health An Interdisciplinary And Intersectoral Issue
The One Health approach has been defined as the collaborative effort of multiple disciplines working locally, nationally and globally to attain optimal health for people, animals and our environment . Health of people, animals and the environment are connected and ABR is acquired not only through human use but can be transferred to humans through selective pressure in the environment. Antibiotic residues in soil, waste water and manure also have a greater impact for resistance than previously thought . Also, while antibiotics as growth promoters in animal production are banned in Europe, without any documented side effects on food availability, quality or price , their use for this purpose is extensive in LMICs.
One Health requires research, surveillance, and interventions across sectors and there is a gap to be bridged between the biomedical, social, environmental and animal sciences . There is a lack of implementation research that tap into the wealth of knowledge that already exists . But some positive efforts are being made. A study in the Netherlands demonstrated a 47% drop in the use of antibiotics in the dairy sector between 2009 and 2015. This example showcases how behaviour change can be achieved with cooperation between stakeholders .
Why You Should Care
Antibiotic resistance has spread around the world, and it’s making some diseases, such as meningitis or pneumonia, more difficult to treat. You might need stronger, more expensive drugs. Or you might need to take them longer. You also might not get well as quickly, or you could develop other health issues.
Each year, an estimated 2.8 million people in the U.S. develop infections that are resistant to antibiotics, resulting in deaths of more than 35,000 people.
Resistance also makes it more difficult to care for people with chronic diseases. Some people need medical treatments like chemotherapy, surgery, or dialysis, and they sometimes take antibiotics to help reduce the risk of infection.
Recommended Reading: Buy Antibiotics For Bv Online
Additional Precautions With Antibiotic Resistant Bacteria
Additional precautions are used when caring for people who are known or suspected to be infected or colonised with highly infectious pathogens .Micro-organisms may be classed as high risk if:
- their transmission route makes them more contagious they may be spread through contact or droplets, or may be airborne
- they are caused by antibiotic resistant bacteria
- they are resistant to standard sterilisation procedures.
Additional precautions are tailored to the particular pathogen and route of transmission. Additional precautions may include:
- use of a single room with ensuite facilities or a dedicated toilet
- dedicated care equipment for that person
- restricted movement of the person and their healthcare workers.
Appropriate Use Of Antibiotics
Preventing an antibiotic-resistant infection starts with the appropriate use of antibiotic medications. Antibiotics are designed to treat bacterial infections, not viral infections like colds or the flu. If you contract a bacterial infection, such as pneumonia or a staphylococcal infection, and a doctor prescribes an antibiotic, its crucial that you take the medicine exactly as your doctor tells you.
Its important not to skip doses and to take all of the medicine, even if you start feeling better. If you stop taking an antibiotic too soon, you can become sick againand some bacteria may survive and develop resistance to the medication.
Never share antibiotic medicines or take antibiotics prescribed for someone else. The antibiotic may not be appropriate for your illness, and taking the wrong medication may delay your treatment and allow the bacteria to multiply.
Don’t Miss: Should You Take Antibiotics For Bronchitis
Take Unused Antibiotics To The Pharmacy For Safe Disposal
If you have leftover antibiotics from previous use, dispose of them correctly by returning them to your pharmacy for safe disposal. Don’t put them down the toilet or sink. There is a risk that antibiotics poured down the sink or flushed down the toilet may pass through treatment systems and enter rivers, lakes and even drinking water supplies. In homes that use septic tanks, antibiotics flushed down the toilet could leach into the ground and seep into ground water. Antibiotics that get into the environment may drive bacteria to become more resistant. Appropriate disposal of antibiotics by the pharmacy minimises this risk. Unused medicines taken to pharmacies are disposed of by specialist waste disposal companies.
Drug Resistance In Fungi
The prevalence of drug-resistant fungal infections is increasing and exasperating the already difficult treatment situation. Many fungal infections have existing treatability issues such as toxicity especially for patients with other underlying infections . Drug-resistant Candida auris, one of the most common invasive fungal infections, is already widespread with increasing resistance reported to fluconazole, amphotericin B and voriconazole as well as emerging caspofungin resistance.
This is leading to more difficult to treat fungal infections, treatment failures, longer hospital stays and much more expensive treatment options. WHO is undertaking a comprehensive review of fungal infections globally and will publish a list of fungal pathogens of public health importance, along with an analysis of the antifungal development pipeline.
You May Like: Can Antibiotics Help With Herpes
Good Hygiene Will Help Stop The Spread Of Bacteria That Make You Sick Keep Your Hands Clean
- Wash them often with soap and water for at least 20 seconds, especially when they are visibly dirty. Use an alcohol-based hand sanitizer when soap and water are not available
- As much as possible, keep your hands away from your:
Be Alert And Take Action

- Be aware of infections and resistance patterns in your facility and community
- Ensure you are notified by the lab immediately when antimicrobial-resistant pathogens are identified in your patients
- Inform patients and families if they have an antimicrobial-resistant infection, as well as sexual partners when appropriate
- Know when to report cases and submit resistant isolates to the health department to identify unusual resistance or treatment failures
To receive email updates about this page, enter your email address:
Links with this icon indicate that you are leaving the CDC website.
- The Centers for Disease Control and Prevention cannot attest to the accuracy of a non-federal website.
- Linking to a non-federal website does not constitute an endorsement by CDC or any of its employees of the sponsors or the information and products presented on the website.
- You will be subject to the destination website’s privacy policy when you follow the link.
- CDC is not responsible for Section 508 compliance on other federal or private website.
CDC.gov Privacy Settings
We take your privacy seriously. You can review and change the way we collect information below.
Cookies used to make website functionality more relevant to you. These cookies perform functions like remembering presentation options or choices and, in some cases, delivery of web content that based on self-identified area of interests.
Don’t Miss: Uti When To Get Antibiotics
Failing To Complete The Course
Patients should always fully complete the prescribed course of antibiotics, every time they are taken. This ensures all bacteria are killed, and so none survive which can subsequently mutate and produce resistant strains. Patients begin to feel well after a few days of taking the medicine, and stop taking them. This is potentially very harmful, as random mutations can occur which can lead to antibiotic resistance. The resistant bacteria reproduce quickly, and the resistance spreads.
Global Action Plan On Antimicrobial Resistance
Globally, countries committed to the framework set out in the Global Action Plan1 2015 on AMR during the 2015 World Health Assembly and committed to the development and implementation of multisectoral national action plans. It was subsequently endorsed by the Governing Bodies of the Food and Agriculture Organization of the United Nations and the World Organisation for Animal Health . To ensure global progress, countries need to ensure costing and implementation of national action plans across sectors to ensure sustainable progress. Prior to the endorsement of the GAP in 2015, global efforts to contain AMR included the WHO global strategy for containment of Antimicrobial Resistance developed in 2001 which provides a framework of interventions to slow the emergence and reduce the spread of AMR.
Also Check: How To Clear A Uti Without Antibiotics
Antimicrobial Stewardship A Safeguard For The Future
Antimicrobial stewardship aims to promote the responsible use of antimicrobials, improve patient outcomes, reduce the emergence of AMR and decrease the spread of infections caused by multidrug resistant organisms . Responsible use should balance the individual´s right to treatment with society´s longer term need for sustained access to effective therapy . The means to achieve this involves the implementation of policies which include evidence-based guidelines for prescriptions . Although it has been suggested that stewardship programmes can reduce antibiotic consumption and resistance, adherence to such programmes is not straightforward in LMICs. Poor countries lack surveillance and adequate infection control and the prohibition of over-the-counter sales of antibiotics is not easily implemented when prescribers are lacking .
A recent systematic review of eight stewardship programmes found no solid evidence of their effectiveness in reducing antibiotic resistance in hospital settings. This is attributed mainly to suboptimal study designs and heterogeneous program features, preventing the pooling of studies .
Education is a key element of stewardship and there are ample indications of knowledge gaps, for example among medical students in choosing therapy. A systematic review of 57 studies revealed poor knowledge among clinicians about the correct prevalence of resistance. They acknowledged the importance of antibiotic resistance but not in their backyard .
Tripartite Joint Secretariat On Antimicrobial Resistance
The political declaration at the UN High Level Meeting on AMR, committed to by Heads of State at the United Nations General Assembly in New York in September 2016, confirmed a strong focus on a broad, coordinated approach that engages all including the human, animal, plant and environmental health sectors. WHO is working closely with FAO and OIE in a One Health approach to promote best practices to reduce the levels of AMR and slow its development.
The Interagency Coordination Group on AMR was convened by the Secretary-General of the United Nations after the UN High-Level Meeting on Antimicrobial Resistance in 2016. The IACG brought together partners across the UN, international organizations and individuals with expertise across human, animal and plant health, as well as the food, animal feed, trade, development and environment sectors, to formulate a plan for the fight against antimicrobial resistance. The Interagency Coordination Group on AMR submitted its report No time to wait: Securing the future from drug-resistant infections to the UN Secretary-General in April 2019. Its recommendations are now being implemented.
Read Also: How To Treat Acne Without Antibiotics
How To Prevent Antibiotic Resistance
We must restrict the use of antibiotics so that we can continue to treat people with serious illnesses, patients who undergo cancer treatment or major surgical procedures that involve a risk of infection. Cancer patients are especially vulnerable to infection during treatment.
Antibiotics must be reserved for patients who are seriously ill, and must be used only by patients who really need them. This will ensure that future generations also have medicines that are effective against infections.
Alerted to this crisis, in May 2015, the World Health Organization adopted a global action plan on antimicrobial resistance with five major objectives: Global action plan on antimicrobial resistance . This urges all countries to act now!
You can also visit WHOs fact sheet on antibiotic resistance